What Is Candida?

So, What is Candida?
What is Candida? It’s a type of yeast that naturally lives in and on the human body. The most common species, Candida albicans, is typically found in the mouth, digestive tract, vagina, skin, and other mucous membranes.
Candidiasis
Candida albicans is normally harmless in small amounts, but an overgrowth can lead to opportunistic infections. These infections are especially common in individuals with weakened immune systems or imbalanced gut flora. Candidiasis can affect various parts of the body, including the mouth, genital areas, and skin, causing discomfort and potential complications if left untreated.
It’s all about – Balance
Healthy bacteria usually keep the yeast in check. Imagine a balanced scale with healthy bacteria on one side and yeast on the other. This balance can be disrupted by factors such as stress, poor diet, weakened immune system, or uncontrolled medical conditions, leading to a Candidiasis overgrowth or infection.
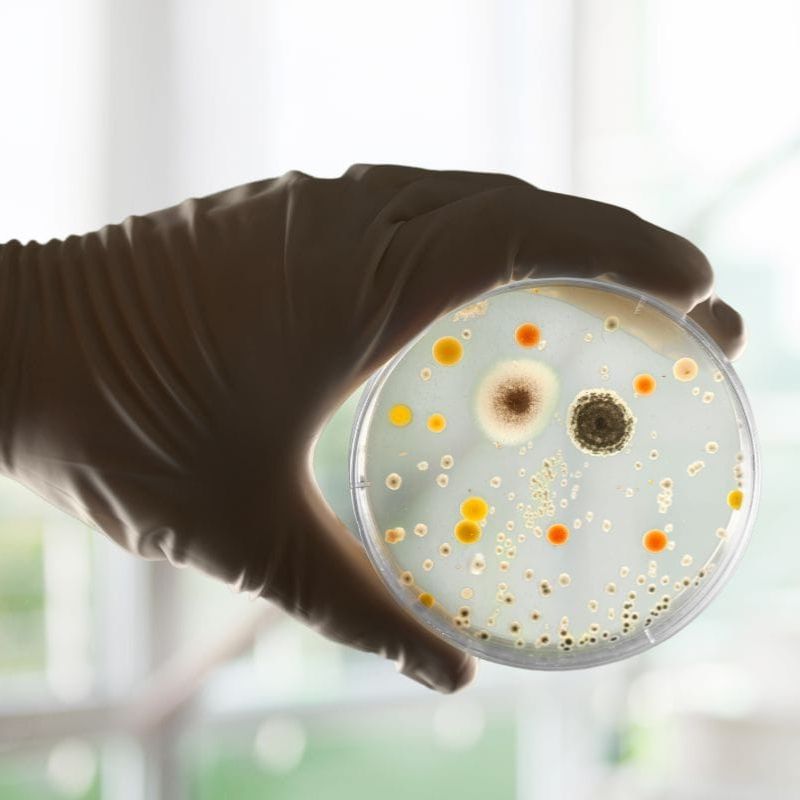
5 Main Species Of Candida
Candida infections in humans are predominantly caused by five main species: Candida albicans, Candida glabrata, Candida tropicalis, Candida parapsilosis, and Candida krusei.
What is Candida albicans?
Candida albicans is the most common species of Candida, with Candida glabrata coming in second place. We’ve seen many stool test reports over the years with these 5 Candida species, but have also commonly encountered more rare Candida species such as Candida kefyr, Candida guilliermondii, and Candida lusitaniae. We’ll discuss Candida albicans a little more below.
Together, these 5 species account for nearly 90% of Candida-related infections (Turner et al., 2014). Each species exhibits unique traits, pathogenicity mechanisms, and host interactions, leading to varied clinical presentations and treatment challenges.
Understanding these differences is critical for effective diagnosis and management. Here are the 5 types we commonly encounter:
Each Candida species has distinct characteristics that influence its ability to cause disease, response to treatment, and clinical outcomes. Continued research is important to improve therapeutic options and combat antifungal resistance.
What Is Candida Auris?
In 2009, a new yeast species belonging to the Candida genus was first identified from the external ear canal of an older patient in a Japanese hospital (Satoh et al., 2009). This strain was named Candida auris, with “auris” derived from the Latin word for “ear” to reflect its site of discovery.
Since its initial identification, Candida auris has rapidly become a global health concern. Almost simultaneously, outbreaks emerged across South Asia, East Asia, Africa, and South America, eventually spreading to over a dozen countries.
In the United States, over 1,460 cases were reported in 2021, and more than 3,000 clinical cases have been documented to date.
Now classified as a superbug, Candida auris has gained recognition as a significant driver of invasive fungal infections worldwide (Ahmad et al., 2021). Its outbreaks have been recorded on every inhabited continent, highlighting its growing role in global public health.
There were 4,514 new clinical cases of C. auris in the United States in 2023. The number of clinical cases has continued to increase since the first U.S. case was reported in 2016.
Particularly alarming is its prevalence in elder care, with outbreaks frequently occurring in hospitals treating older, critically ill patients. These infections are associated with high mortality rates, largely due to C. auris’s multi-drug resistance and ability to spread within healthcare settings. As a result, the Centers for Disease Control and Prevention (CDC) have designated Candida auris as a serious global health threat.
Candida Albicans
What is Candida albicans?
Candida albicans is the most prevalent yeast species among over 100 types of Candida that can affect humans. It is often viewed as a “commensal” organism, meaning it typically co-exists peacefully within the body without causing harm under healthy conditions.
This delicate balance is maintained by our body’s natural defences, including our immune system, stomach acidity, saliva, and the competitive presence of other microorganisms. However, under certain conditions—such as immune suppression or microbial imbalance—Candida albicans can transition from a benign state to a pathogenic (disease-causing) one, leading to different kinds of infections.
How Common is Candida albicans?
According to the Centers for Disease Control and Prevention (CDC), Candida albicans is the most common species of Candida responsible for infections in humans. Colonisation of C. albicans often begins early in life, with exposure occurring during childbirth, nursing, or through food (Jenkinson et al., 2002). This yeast can colonise various parts of the body, including the skin, oral cavity, gastrointestinal tract, and vaginal mucosa.
Studies reveal that up to 40% of healthy adults carry C. albicans in their oral cavity, while 20–25% of women harbor it in their vaginal tract (Jenkinson et al., 2002). While colonization is typically harmless, disruptions in the microbiome or immune system can lead to opportunistic infections.
Key Articles
The Growing Threat of Candida Infections
Candidiasis is caused by Candida species, which naturally reside on the skin, mucous membranes, and within the body without causing harm. However, uncontrolled Candida growth can lead to invasive infections, such as candidemia, which affect multiple organs and can be life-threatening (Kullberg and Arendrup, 2015).
Key Points About Candida Infections:
What Types of Candida Albicans Infections (Candidiasis) Exist?
Each year, millions of people are affected by Candida albicans and other Candida species overgrowth. Although it can affect any region of the body, it frequently results from an imbalance in our gut flora. It might be challenging to get rid of the symptoms of Candida unless you correct the gut imbalance.
According to recent studies, once Candida is in its pathogenic state and invades our body through gastrointestinal permeability (leaky gut), it can cause diseases ranging from debilitating superficial to life-threatening systemic infections. (Basmaciyan et al., 2019)
Some Of The Common Types of Infections Caused by Candida Albicans Include:
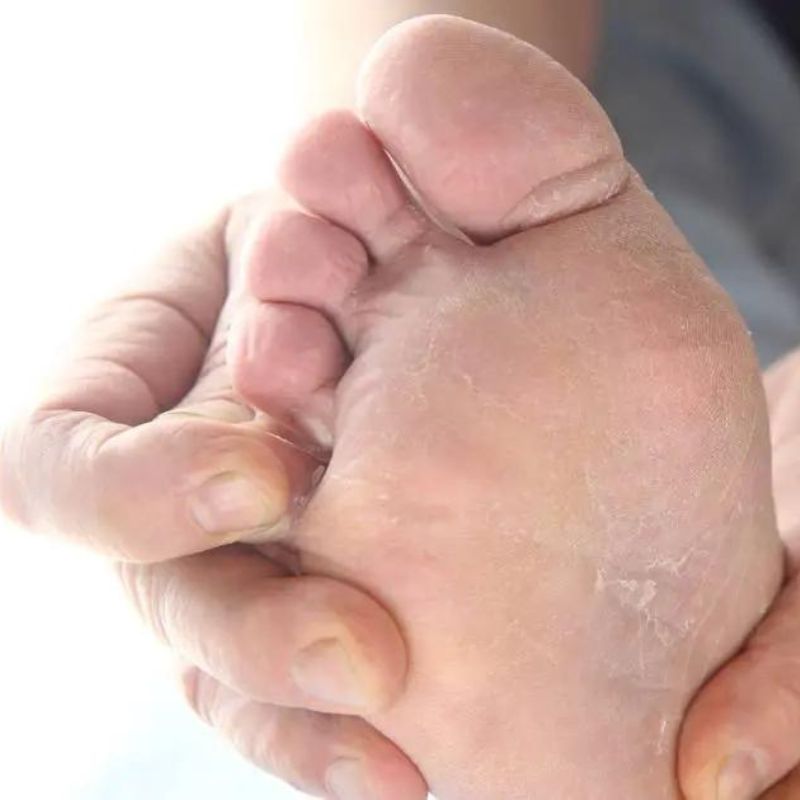
Athlete’s Foot
Athlete’s foot is one of the most prevalent superficial fungal infections, affecting an estimated 15-25% of the global population at any given time (Ameen, 2010). It is caused by dermatophytes, particularly species of Trichophyton.
The infection typically starts between the toes and can spread to the soles and sides of the feet. Warm, moist environments, like gym showers and locker rooms, are common sources of transmission. Athlete’s foot often coexists with nail fungus, as both infections thrive in similar conditions and are caused by overlapping fungal species.

Children’s Yeast Infections
Children’s yeast infections are also common. Children can develop Candida yeast infection in a variety of places. Infants can develop diaper rash, while older children can develop a variety of Candida infections like adults. Children are often attracted to sweet and sugary foods linked with Candida and fungal overgrowth

Invasive Candidiasis
A severe infection that targets your whole body, specifically your blood, bones, brain and heart. The condition known as invasive candidiasis is characterised by the introduction of Candida into the bloodstream, which can result in severe problems.
Invasive candidiasis (IC) is a serious infection caused by several Candida species, and the most common fungal disease in hospitals in high-income countries. (Soriano et al., 2023)

Oral Thrush
Oral thrush commonly affects the inside of a person’s mouth. White patches on the tongue and inner cheeks are the telltale signs of oral thrush, which is a fungal illness that affects the human mouth.
An overgrowth of yeast may form on on inside of the mouth including the throat. Candidiasis is a condition that can affect the oesophagus and causes discomfort and trouble swallowing. Oral thrush may appear as white, raised bumps.

Male Yeast Infection
Male yeast infection is an often under diagnosed condition. Men can also develop Candida infection of their penis.
In our clinical experience, not many men want to talk about it, let alone get help from their doctor. There are different forms of penile yeast infections involving Candida albicans.

Nail Fungus
Nail fungus is one of the world’s most common fungal infections. These infectionsof the nail are caused by a variety of fungal species, including dermatophytes, molds, and yeasts. Dermatophytes are responsible for most cases of nail fungus however, particularly in toenails. The global prevalence of nail fungus is about 5.5%, according to recent studies, making it a common fungal infection (Leung et al., 2020).

Vaginal Yeast Infection
Vaginal yeast infections are also known as vaginal thrush or vaginal candidiasis. Itching, discomfort, and discharge are all symptoms of genital yeast infection, which is a common condition among females.
Vaginal yeast infection occurs when these yeast multiply inside the vagina causing an infection.
Is Candida a Sexually Transmitted Disease?

Candida albicans can be transmitted sexually, although is not considered an STI (STD, sexually-transmitted disease) because you can get it without having sex.
Fungal infection can passed on through sexual contact. This yeast is naturally present in various parts of the body, including the mouth, digestive tract, and genital area. The balance of Candida and healthy bacteria typically regulates the yeast growth. (Pérez et al., 2021)
Imbalances in this equilibrium can cause an overgrowth of Candida and subsequent infections. Factors like antibiotics, hormonal changes, a weakened immune system, or a high-sugar diet can cause this imbalance.
While sexual activity does not directly cause Candida overgrowth or infections, although it can affect the balance of yeast and bacteria in the body.
Engaging in sexual activity can introduce new bacteria to the genital area, potentially leading to yeast overgrowth. To prevent Candida overgrowth, it’s important to maintain good hygiene, eat a clean and healthy diet, and consider taking probiotics.
Can a Male Get Candida?
Most people associate yeast infection with women, but in my experience they can affect can anyone, including men. If untreated, a penile yeast infection can lead to serious complications if it spreads to the bloodstream and could cause invasive candidiasis. (Arya et al., 2023)
Penile yeast infections can cause discomfort and pain, including balanitis. Over-the-counter and prescription medications can effectively treat them, depending on the severity. Proper hygiene practices can help reduce the risk of infection.
Most penile yeast infections can be cleared up with OTC medications, though sometimes prescription treatments are necessary. Basic preventive measures, such as maintaining good hygiene, can help avoid this common condition.
Men’s Yeast Infections
Candida Symptoms

How Does Candida Cause Symptoms?
As the Candida population increases, it can potentially produce an increasing amount of harmful metabolites. Uric acid, ammonia, and acetaldehyde are some of these toxic by-products, and so are the specific toxins produced by Candida, the mycotoxins. The symptoms these chemicals can produce may manifest as headaches, mental fog, weariness, and many kinds of digestive issues.
These yeast can produce long branches (hyphae) that can penetrate your soft tissue when it transforms into a fungus. These can then enter your digestive tract, mouth, vaginal area and other areas of your body and release these same waste products into the surrounding tissue.
Candida employs various methods of pathogenicity (the ability to cause disease), it escapes the body’s immune responses, physical change (changes from yeast-to-hyphae), and invasion. Research has shown these methods are all further supported by the production of adhesion molecules and different types of enzymes that can dissolve things, like cell membranes. (Wilson et al., 2009)
Your immune system responds to these metabolites, which can result in symptoms like inflammation, allergies, and many different kinds of health issues.
Candida Causes and symptoms

Candida Overgrowth
Understanding Candida Overgrowth
Candida overgrowth refers to an excessive proliferation of Candida yeast within the body. While Candida is a natural part of the body’s microbiome—commonly found in the gastrointestinal (GI) tract, mouth, and on the skin—its overgrowth can lead to a variety of health issues.
This imbalance often occurs when factors such as antibiotics, high sugar or refined carbohydrate intake, a compromised immune system, or chronic stress disrupt the natural equilibrium of microorganisms in the body.
Symptoms of Candida Overgrowth
The symptoms of Candida overgrowth can manifest throughout the body and vary widely. Common signs include:
Challenges in Diagnosis
Diagnosing Candida overgrowth can be challenging due to the overlap of symptoms with other conditions. Healthcare professionals may rely on a combination of clinical evaluations and laboratory tests, such as stool analysis, blood tests, or swabs, to identify Candida overgrowth accurately.
Treatment and Prevention
Effective treatment of yeast overgrowth typically involves a multifaceted approach:
Preventive measures can also play a crucial role in minimising the risk of Candida overgrowth:
By addressing both the root causes and symptoms, individuals can restore balance to their microbiome and reduce the likelihood of Candida overgrowth, improving overall health and well-being.

Candida Cleanse
Understanding Candida Cleansing
The human digestive tract naturally hosts Candida yeast as part of the normal microbiota, with Candida albicans being the most common species. In a healthy, balanced gut, Candida albicans typically coexists without causing any harm. However, research suggests that an overgrowth of Candida albicans in the gut can contribute to various digestive and systemic health issues. Let’s explore what a Candida cleanse involves and what it means for overall health.
Candida albicans is a fungal species that colonizes multiple regions of the body, including the ears, nose, throat, skin, gastrointestinal (GI) tract, and vaginal tract. It is estimated that Candida albicans is a normal part of the gut flora in about 50–60% of the population (Talapko et al., 2021). While its presence is normal, its overgrowth can disrupt the microbiome, leading to health concerns.
What Does “Candida Cleansing” Mean?
The term “Candida cleanse” is widely used in natural medicine to describe protocols aimed at addressing Candida overgrowth. However, some healthcare professionals argue that this term can be misleading and prefer evidence-based terms such as “Candida treatment” or “Candida protocol” to emphasize scientifically supported strategies for addressing fungal overgrowth.
It’s worth noting that while Candida overgrowth is a genuine health issue, claims about its prevalence can often be exaggerated in certain online sources or by practitioners engaging in fear-based messaging. For example, some interviews with healthcare professionals claim that Candida affects up to 90% of women, a figure that lacks support from reputable research.
Medical experts and reputable health websites caution against accepting such exaggerated statistics, urging individuals to approach information about Candida critically. Misinformation can lead to unnecessary alarm or reliance on unproven remedies.
Key Takeaways

Candida Diet
What Is Candida Diet?
The Candida Diet focuses on eliminating foods that fuel Candida growth, particularly refined carbohydrates and processed foods, while incorporating nutrient-dense, whole foods that support a balanced microbiome. Rather than rigidly adhering to an “anti-Candida diet,” adopting a sustainable, anti-processed foods approach often yields better long-term results.
This way of eating is best seen as part of a broader strategy for gut health. For sustained results, consider transitioning to the Foundation Diet after completing a gut cleanse. This involves identifying which foods are best suited for your gut while minimising or avoiding those that trigger symptoms or contribute to imbalances.
Candida Diet Approach
Key Take-Aways
Candida Diet Food List
Transitioning to a sugar-free, whole-foods diet is one of the most effective ways to alleviate symptoms of Candida overgrowth and bacterial dysbiosis. This dietary approach aims to restore gut balance by eliminating foods that feed Candida and promoting those that support a healthy microbiome. Let’s look at a few pages that dive deeper into the principles and benefits of the Candida Diet, and how it can help improve your overall health.
The Ultimate Candida Cleanse System
Restore gut balance naturally with the Ultimate Candida Cleanse System — a complete, professional-grade gut health solution.

This all-in-one system developed by naturopath Eric Bakker, N.D., combines two in-depth books — The Ultimate Candida Cleanse Program and The Ultimate Candida Cleanse Guide — along with the Yeastrix Gut Restore Kit, featuring targeted antifungal, probiotic, and enzyme formulations. Together, they deliver a structured, step-by-step approach to eliminating Candida overgrowth, rebalancing your gut microbiome, and rebuilding healthy digestion from the inside out — your foundation for lasting energy, comfort, and vitality.
To achieve real, lasting results, you need more than just a plan — you need the right support. That’s why Eric Bakker created Yeastrix, a professional-grade supplement range launched in 2025 to work hand-in-hand with his new Candida Cleanse Program. Each Yeastrix formula targets a key stage of gut recovery — helping restore microbial harmony, enhance digestion, and support long-term wellness.
If you’re ready to take control of your health and finally feel like yourself again, the Ultimate Candida Cleanse System gives you everything you need — expert guidance, a proven roadmap, and powerful natural support that truly works.

The Vaginal Yeast Infection Treatment Program
Many Candida species are becoming increasingly resistant to anti-fungal drugs. Fungal-related health problems have become a hidden epidemic and are increasing. Women are increasingly looking for more drug-free and natural ways of overcoming their personal health challenges. With the latest research into natural medicines and fungal/bacterial overgrowth in our new yeast infection treatment program, we can offer many supportive solutions. The Vaginal Yeast Infection Treatment Program.
Created by a naturopath with years of specialist clinical and research experience in the field of Candida yeast infections, SIBO, and other gut-related health problems such as IBD and IBS.
Thanks for viewing this page, please leave a comment if you wish.