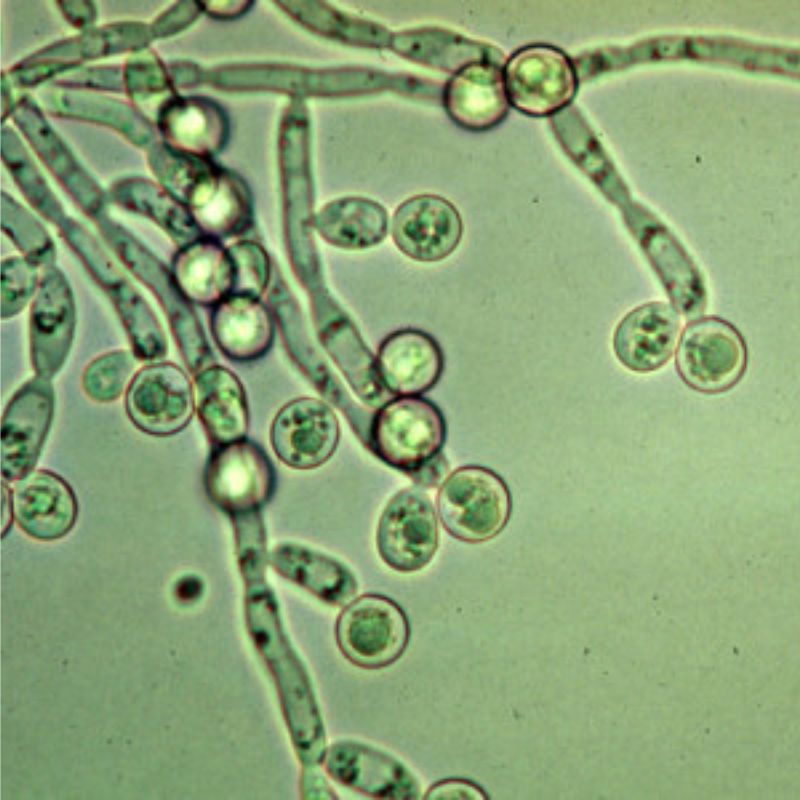
Biofilm Explains Why Candida and Yeast Infection Are Hard To Beat
A clear, clinically grounded overview — and your starting point for understanding why Candida can be so persistent.
If you’ve been dealing with Candida and feel like you’re going in circles, this is the page to start with. Biofilms are often the missing piece.
These fungal biofilms help explain:
This guide pulls everything together in plain English — and then points you to deeper articles so you can go further.
Don’t worry, this page is not as complicated as it seems! I’m here to make understanding Candida biofilms a breeze. Candida species might at first seem harmless, but can cause significant health concerns if it gets out of control.
Table of contents
- Biofilm Explains Why Candida and Yeast Infection Are Hard To Beat
- What Is a Candida Biofilm?
- Why Biofilms Matter
- Where Biofilms Form
- The 4 Stages of Biofilm Development
- What Makes Biofilms So Tough?
- Not All Candida Is The Same
- Candida Doesn’t Always Act Alone
- Why Candida Treatment Can Be Difficult
- Why Candida Treatment Can Be Difficult
- Start Here – The Full Biofilm Series
- Key Take-Aways
- Final Word
What Is a Candida Biofilm?
A Candida biofilm is a structured community of yeast cells that sticks to a surface and protects itself with a self-made coating.
In simple terms:
This matrix acts like a buffer — reducing the effectiveness of antifungals and immune attack.
Why Biofilms Matter
Once Candida forms a biofilm, everything changes. You’re no longer dealing with loose yeast cells.You’re dealing with a protected system.
That can lead to:
This is why biofilms are strongly linked to chronic Candida issues.
Where Biofilms Form
Candida prefers mucosal surfaces in the body. The most common locations include:
In clinical settings, Candida biofilms can readily form here:
Once attached, Candida can build a stable biofilm that acts as a reservoir.
The 4 Stages of Biofilm Development
Candida biofilms don’t appear overnight. They develop in stages:
- Adhesion — yeast sticks to a surface
- Growth — cells multiply
- Maturation — a structured biofilm forms
- Dispersion — cells break off and spread
That last step — dispersion — is a big reason Candida infections come back and can easily spread.
What Makes Biofilms So Tough?
Several factors work together:
It’s not one mechanism — it’s a layered defence system.
Not All Candida Is The Same
Did you know that all Candida species behave differently, just like humans?
The most common ones include:
These differences do matter, because they influence:
Candida Doesn’t Always Act Alone
In many cases, Candida is part of a mixed microbial community.
This often means:
This adds another layer of complexity — especially when it comes to gut and vaginal health.
Why Candida Treatment Can Be Difficult
Standard antifungal treatments often struggle because:
In clinical settings, especially with devices → Removing the source is often essential
New antifungals show promise, but → No single drug reliably eliminates biofilms in all cases
Why Candida Treatment Can Be Difficult
Candida biofilms are:
They are not “invincible” — but they do require a more thoughtful approach.
Start Here – The Full Biofilm Series
This guide is your overview of the biofilm articles on this site.
To really understand Candida biofilms — and why they can be so persistent — I highly recommend working through the full series below.
Each article builds on the last, so you can go from simple understanding to deeper insight, and then practical application.
1. Candida Biofilms Explained
Why your infection keeps coming back
Start here. This article breaks things down in plain English and gives you the big picture.
You’ll learn:
• What Candida biofilms actually are
• Why they matter for your health
• Where they tend to form in the body
• Why symptoms improve… then return
2. Biofilm Stages
The 4 phases of Candida biofilm development fully-explained
Once you understand the basics, the next step is seeing how biofilms actually develop. We go a bit deeper into the science here. You’ll also find several scientific references on this page.
This article walks you through the full biofilm lifecycle, step by step.
You’ll learn:
This is the piece that connects formation → persistence → relapse
3. Inside Candida Biofilms
Structure, species differences and survival mechanisms
Now we go deeper. This article explains what’s happening inside the biofilm and why it behaves the way it does.
You’ll learn:
4. Why Candida Biofilms Are So Hard to Treat
And what actually works
Finally, we bring it all together.
Understanding the clinical reality. This is where you understand why treatment can be difficult — and what actually makes a difference.
You’ll learn:
How to Use This Series
If you’re short on time:
If you want a deeper understanding:
If you’ve been dealing with long-term or recurring Candida:
Key Take-Aways
Final Word
Candida biofilms are not complicated once you understand them properly. But they do require a shift in thinking. This series is designed to give you that shift — step by step. If you’ve struggled with persistent Candida, this is not something to ignore! But it’s also not something to fear.
Biofilms are:
The goal is not just to “kill yeast.” It’s to understand how it survives — and why.

Eric Bakker N.D.
Greetings! I am a naturopathic physician from New Zealand. Although I’ve retired from clinical practice since 2019 after 34 years of clinic. I remain passionate about helping people improve their lives. You’ll find I’m active online with a focus on natural health and wellbeing education through my Facebook page, Reddit page and YouTube channel, including this website.





