
Vaginal Yeast Infection
Vaginal yeast infections are a common yet often uncomfortable condition experienced by many women at some point in their lives. This fungal infection occurs when there is an Candida overgrowth of yeast, most commonly Candida albicans, in the vaginal area. While primarily affecting women, men can also contract yeast infections, typically as penile yeast infections from sexual contact with an infected partner.
Vaginal yeast infections are more commonly experienced by women than any other genital yeast infection (NIH). According to estimates, over half of women worldwide experience more than one episode of vulvovaginitis at some point in their lives, making up about 75% of all women. (Brown 2020).
This page on vaginal yeast infection is dedicated to those women, it is comprehensive and has links to many other prominent pages and natural health programs on this website.

Our Focus on Women’s Yeast Infections
Maintaining optimal vaginal health starts with understanding the causes, symptoms, and treatment options for vaginal yeast infections. While medical treatments can be effective, addressing lifestyle factors and underlying health conditions is key to preventing recurring infections.
For those seeking natural solutions, this website offers dedicated resources on managing vaginal yeast infections. Women make up over 75% of the patients I treated in my clinic, with many facing challenges related to hormonal health, digestion, and the urinary or reproductive systems. That’s why much of the focus here is on chronic vaginal yeast infections and related genito-urinary conditions.
The Yeast infection Specialist
For many years, our clinic specialised in treating yeast infections, with a particular focus on the unique challenges faced by women. While vaginal yeast infections were the most common concern, we also addressed yeast-related conditions affecting the skin and nails, which are discussed in other sections of this websites
By the mid-1990s, we began achieving remarkable results with the yeast-cleansing protocols we developed. These protocols continued to evolve, leading to advanced Candida and SIBO (Small Intestinal Bacterial Overgrowth) treatment strategies by the late 1990s and further refinements throughout the early 2000s.
Candida Crusher
In 2013, I published Candida Crusher, a comprehensive guide that laid the groundwork for our highly effective vaginal yeast infection treatment protocols.
A decade later, candida.com builds upon this foundation, offering the latest research-backed and natural approaches to overcoming yeast infections. With our NEW Yeast Infection Treatment program, along with cutting-edge insights for 2025, this website serves as my second book on Candida, a culmination of (almost 40 years) clinical experience, research experience, and success in natural medicine.
This page takes a deeper close look into the topic of vaginal yeast infections than just about any other website you’ll find, exploring their causes, symptoms, and much more. We’ll begin with a brief look at the vaginal microbiome before moving on to address the key factors behind vaginal yeast infections and how to effectively manage them.
The Vaginal Microbiome
The vaginal microbiome plays a crucial role in maintaining vaginal health and preventing infections. Unlike other body areas, such as the mouth, throat, and gut, the vaginal microbiome is much less diverse, with Lactobacillus species dominating (Human Microbiome Project Consortium 2012).
Protective Functions of the Vaginal Microbiome
Maintaining a healthy and balanced vaginal microbiome is essential for preventing infection and managing symptoms like itching or irritation. Hormonal changes, lifestyle factors, and ethnic differences all influence microbiome diversity, which in turn impacts vaginal health.
Let’s now look at vaginal yeast infection symptoms, the common and not-so-common:
Vaginal Yeast Infection Symptoms

A healthy vagina naturally contains a balance of bacteria and yeast cells. When this balance is disrupted, typically by an overgrowth of Candida yeast, symptoms can develop rapidly.
The symptoms of a vaginal yeast infection can vary, both physically and emotionally, and can sometimes escalate quickly.
In my years of practice, I have encountered many ways that vaginal yeast infection symptoms can present. While common signs are more typical, there are also less common symptoms that may appear. It’s also important to note that various types of vaginitis, which is vaginal inflammation, can have overlapping symptoms.
For example, bacterial vaginosis is a bacterial infection that can cause symptoms like itching, swelling, and irritation, similar to those seen in yeast infections.
It’s also possible for the infection to affect areas beyond the vagina, such as the vulva (the outer skin around the vagina) or the perineum (the skin between the vagina and anus).
Vaginitis, Vulvitis, And Vulvovaginitis
Read: Vaginitis Symptoms, Causes, Treatments, and Prevention.
Because yeast infections share symptoms with other conditions, it is crucial to differentiate them. However, itching and discomfort in the vaginal or vulvar areas are usually the most common and distinct symptoms of a vaginal yeast infection, making it an important indicator for diagnosis and treatment.
Vaginal Yeast Infection Discharge
Vaginal thrush is often accompanied by a painful, frustrating discharge. Typically creamy, it may have curd-like strands and cause discomfort that affects both sexual health and emotional well-being. Studies show that women with recurrent vaginal candidiasis are more likely to experience clinical depression, low self-esteem, and heightened stress levels.
Although many women feel embarrassed, thinking that vaginal thrush reflects poor hygiene, it can affect women from all walks of life, regardless of cleanliness or lifestyle. For some, yeast infections are rare, while others experience them regularly. Key symptoms of vaginal yeast infections include persistent itching and irritating discharge, which can be distressing.
Key Features of Vaginal Yeast Infection Discharge:
If the discharge doesn’t align with the typical signs of a yeast infection, it’s important to consult a healthcare provider to rule out other causes.
Recurrent Vulvovaginal Candidiasis (RVVC)
For up to 15-20% of women, yeast vulvovaginitis can become a recurring issue. When a woman experiences four or more yeast infections in a single year, this is classified as recurrent vulvovaginal candidiasis (RVVC). Recurrent infections can be distressing and frustrating, often requiring a deeper investigation into potential underlying causes (Pan et al., 2023).
Candida Forms Biofilms
Studies using animal models have shown that Candida albicans can form biofilms on the vaginal lining, but the role of these biofilms in human vaginal yeast infections (VVC and RVVC) has been discovered through recent studies (Rodríguez-Cerdeira. etal., 2020).
Recent research examined vaginal tissue samples from otherwise healthy women with recurrent infections (RVVC) to understand how Candida grows and affects the vaginal lining.
Key findings from the study include:
This suggests that biofilms may play a significant role in the persistence of recurrent vaginal yeast infections.

Vaginal Itching, Irritation, And Burning
Vaginal yeast infection can cause significant discomfort and disruption, with symptoms that are usually hard to ignore. Many women find itching, burning, and irritation in the vaginal and vulvar areas are some of the most common (and embarrassing) signs.
Pain during urination or sexual activity may also occur, along with a thick, white vaginal discharge. For men, symptoms of a penile yeast infection can include redness, itching, or a rash on the penis.
Treating a vaginal yeast infection can relieve symptoms within a few days. In more severe cases, it may take longer and be recurring. You may well be interested in learning more about the best natural treatment of vaginal yeast infections.
Although yeast infections can be uncomfortable, they are typically manageable with the right treatment. However, in severe or recurring cases, it’s crucial to address underlying factors that may contribute to the infection. Factors like antibiotic use, hormonal changes, diabetes, or a weakened immune system can all play a role in triggering an overgrowth of yeast. Lifestyle factors such as poor diet rich in ultra-processed or junk foods, wearing tight, synthetic clothing or poor hygiene practices can further increase the risk.
Medical treatments for vaginal yeast infections usually involve antifungal medications, which are widely available over-the-counter or by prescription. These come in various forms, including creams, ointments, tablets, and suppositories. Common antifungal medications include clotrimazole, miconazole, and fluconazole. For men, antifungal creams can effectively treat penile yeast infections. Following the full course of treatment is essential to ensure the infection is fully eradicated.
The Key Symptoms Of Vaginal Yeast Infection

Vaginal Itching and Scratching: A Path to Infection
Persistent vaginal itching is not only uncomfortable but can also lead to further complications if left unaddressed. Scratching the affected area, particularly if the skin is already sensitive or inflamed, can create tiny breaks in the skin.
These open areas make it easier for harmful bacteria to grow and worsen the symptoms, causing a secondary infection. Inflammation can also spread to nearby tissues, such as the opening of the urethra, potentially causing additional discomfort or infections (Chiu 2017).
While severe complications are rare, they are more likely in individuals with weak immune systems, such as those undergoing cancer treatment or living with conditions like hepatitis or HIV. In such cases, the inflammation can intensify and spread to surrounding areas more extensively (Murphy et al., 2016).
No Increased Risk During Pregnancy

Some websites claim that for pregnant women, vaginal yeast infections pose additional health concerns. They say women’s yeast infections can increase the risk of complications like premature labor, miscarriage, or preterm birth.
A recent study however reviewed the scientific literature on vulvovaginal yeast infections in pregnancy and their impact on perinatal outcomes.
No strong evidence was found linking these infections, whether the patient has symptoms or not, to pre-term birth, low birth-weight, or eight other adverse outcomes (Gigi et al., 2023).
One concern however, is that yeast infections can be transmitted to a newborn baby during delivery. This can result in conditions such as oral thrush (irritation of the tissues lining the baby’s mouth) or diaper rash, also known as nappy rash.
The Stigma Around Yeast Infections
Embarrassment about vaginal health often delays treatment, prolonging symptoms and increasing the risk of severe infections or transmission to others. Open communication with doctors and partners is key to breaking this stigma, ensuring timely care, and preventing complications. Let’s look at diagnosis:
Vaginal Yeast Infection Diagnosis

Diagnosing a vaginal yeast infection typically begins with a review of your medical history, including any prior yeast infections or sexually transmitted infections (STIs). Your doctor may perform a pelvic examination to check for signs of inflammation, redness, and swelling in the cervix and vaginal walls, which can help identify potential causes of vaginal discharge.
If necessary, your doctor may take a vaginal cell sample (smear test) for lab analysis to confirm the diagnosis and rule out other conditions like bacterial vaginosis (BV), which can present similarly to a yeast infection. For women with recurrent infections, lab tests are often recommended.
If available, pH paper may be used to help identify the infection. It’s also helpful to determine the specific Candida strain involved, as some strains like Candida glabrata may not respond well to common antifungal treatments like fluconazole.

Diagnostic Tests for Candida Infections
To confirm the presence of Candida in a patient, several diagnostic tests are commonly used (Jeanmonod et al., 2024). These tests help differentiate Candida infections from other vaginal conditions.
Frequently used methods to detect the presence of Candida include:
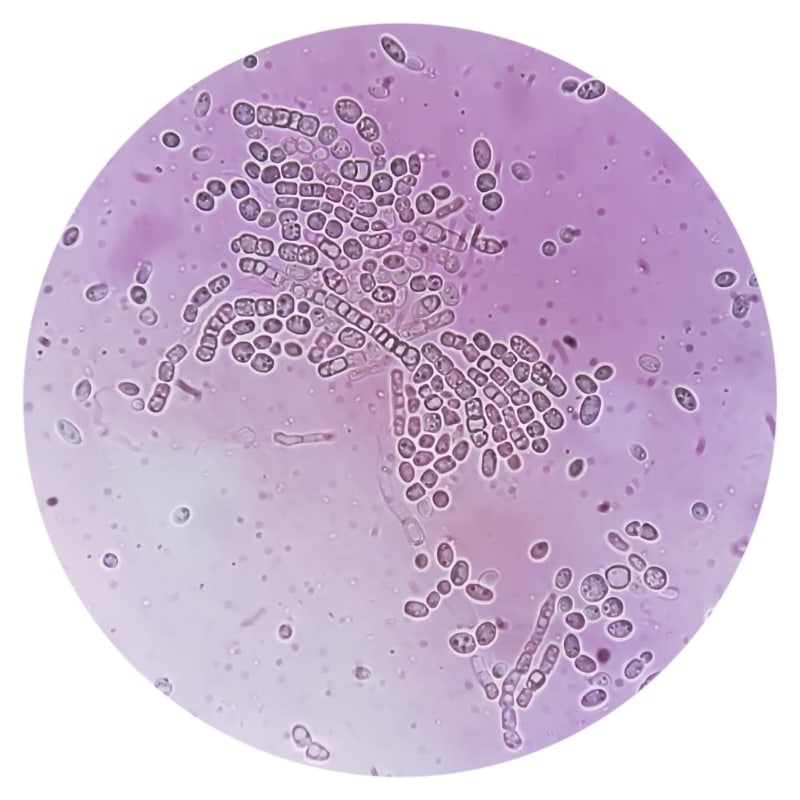
Key Findings in Candida Infections
Characteristic signs of Candida infections can be identified during microscopic examination:
Additional Considerations
When to Avoid Routine Cultures
By utilizing these diagnostic methods, doctors can accurately diagnose Candida infections and ensure appropriate treatment.
Home Diagnosis: More Problematic Than Home Treatment
From my experience, one of the most significant concerns with home treatment and self-diagnosis is the risk of misidentifying the real issue. While medical professionals typically discourage self-diagnosis and self-treatment, there are valid reasons for this caution, especially when dealing with conditions like vaginal yeast infections. If you are unfamiliar with the symptoms or have never had a yeast infection before, it’s easy to misdiagnose.
The Challenge of Home Diagnosis:
For these reasons, I always recommend women consult their primary healthcare practitioner if they’re uncertain about symptoms like itchiness, discharge, or irregular cycles.
In many cases though, women will have already seen their doctor, especially if they have a history of recurrent vaginal infections.
What Causes Vaginal Yeast Infections
Vaginal yeast infections often occur when the natural balance of microorganisms in the vagina is disrupted. Candida albicans, which normally lives harmlessly in up to 20% of women, can overgrow due to factors like pregnancy, antibiotics, steroids, or oral contraceptives.
Medical conditions such as diabetes or autoimmune diseases, which weaken the immune system, also increase the risk, as do genetic predispositions that affect the body’s ability to combat Candida.
Lifestyle factors like stress, tight or synthetic clothing, non-breathable underwear, and poor hygiene habits can further contribute to yeast infections. Even external sources, such as sexual contact with a partner who has a yeast infection, can introduce yeast to the vaginal area. Understanding these triggers is key to prevention and maintaining a healthy balance. Key causes include:
Article Of Interest: 10 Most Common Causes Of Vaginal Yeast Infections.
Break The Cycle Of Recurring Vaginal Yeast Infections
According to some researchers, 15 to 20 percent of all women worldwide suffer from recurrent and chronic vaginal candidiasis. (Denning 2018)
Antibiotics Can Be A Key Trigger

Your doctor might suggest that recurrent yeast infections could be linked to an underlying medical condition, such as diabetes, immune dysfunction, or hormonal imbalances, and recommend more aggressive treatments like antifungal medications or even antibiotics. However, in many cases, the truth is quite the opposite.
Antibiotics are often a trigger for yeast infections, as they disrupt the delicate balance of beneficial bacteria in the vaginal and gut microbiomes, allowing Candida to thrive unchecked.
One study involving more than 30,000 women shows a significant increase in the risk of developing vaginal candidiasis following the use of the antibiotics studied (ciprofloxacin, ofloxacin, norfloxacin, cefixime, azithromycin and fosfomycin) (Wilton et al., 2003).
Vaginal Yeast Infection Treatments
Medical Treatment Of Yeast Infection

Doctors often recommend antifungal treatments for vaginal yeast infections, usually combining oral drugs like fluconazole with topical creams or suppositories.
These treatments can vary in duration, from a single dose to several days, depending on the severity of the infection. However, oral antifungals like fluconazole are typically avoided during pregnancy, with safer alternatives like clotrimazole prescribed instead.
It’s important to follow the correct dosage and avoid alcohol or sugar-heavy diets during treatment, as these can hinder recovery. For mixed infections involving bacteria or other pathogens, combination therapies may be advised.
While over-the-counter (OTC) antifungal remedies are popular, they are not always used correctly. Studies show that some women self-diagnose and treat symptoms that may not even be caused by Candida. (Ryan-Wenger et al., 2011).
Naturally, if symptoms persist, it’s always essential to consult a healthcare professional for an accurate diagnosis and to address underlying causes, as treating symptoms alone often leads to recurrence.
Unlike pharmaceutical antifungal drugs, natural remedies like those in Yeastrix formulations do not contribute to fungal resistance, offering a safer and highly effective alternative for long-term management of yeast infections. Learn more at www.yeastrix.com.
Some medical websites dismiss natural remedies for Candida yeast infections, arguing that they don’t work. However, there is a significant body of research supporting the effectiveness of various natural treatments.
Some common opinions you may find online include:
Interestingly, in obstetrics and gynaecology, Lactobacilli species are used to restore the physiologic vaginal microbiota in order to treat bacterial vaginosis and vulvovaginal candidiasis (VVC) and can even help prevent preterm birth (Buggio et al., 2019).
Rising Resistance to Antifungal Drugs:
What these websites often overlook is the increasing resistance to pharmaceutical antifungal drugs, especially fluconazole, used for decades to treat Candida infections. About 7% of all Candida blood samples tested at CDC are resistant to the antifungal drug fluconazole.
Since the late 1990s, mutations in Candida albicans have made this drug less effective, and in some cases, it may even be harmful. Recent studies mention “the mining of natural products” when it comes to new antifungal drugs (Lee et al., 2020).
In this website, we explore various research and studies on natural remedies such as apple cider vinegar, garlic, probiotics, coconut oil, and tea tree oil. You’ll be able to decide for yourself whether these treatments are as ineffective or mythical as some claim, based on some of the most recently available scientific evidence. It’s time to look beyond personal opinions, hypothesis, and evaluate the real facts.
Updated Natural Yeast Infection Treatment

In 2013, my book Candida Crusher introduced a three-stage program to address chronic vaginal yeast infections. Over the next six years, before retiring from clinical practice in 2019, I continued to refine this approach through extensive research and hands-on experience.
With over 30 years of expertise in managing Candida overgrowth and persistent vaginal thrush, I’ve developed a comprehensive protocol that consistently delivered outstanding results.
Recent advancements in vaginal microbiome research have inspired me to expand and enhance the original program. What began as a three-stage approach has evolved into a more complete and effective four-stage protocol, designed to provide deeper cleansing, better balance, and long-term relief from yeast infections.
3 Months Minimum for Chronic Cases

For chronic or recurring vaginal thrush, I strongly recommend committing to this program for at least 12 weeks (3 months). This duration is the minimum, and essential for fully restoring a healthy vaginal microbiome and reducing the likelihood of relapse.
By following our Ultimate Candida Cleanse Treatment Program, alongside the Candida diet and a few high-quality specialised Candida supplements, you can achieve the same results as the many women helped through this protocol. Over the years, our clinic has successfully treated even the most severe, long-standing cases of vaginal thrush, and I’m confident this approach can work for you.
This protocol is especially beneficial for:
By addressing root causes and restoring balance, our protocol offers a sustainable and effective path to healing. If you’re ready to commit, you’ll be amazed at how quickly your body can respond. Take the next step and commit to our vaginal yeast infection treatment program.
The 4-Steps to Vaginal and Gut Cleansing and Balancing
The 4-step yeast infection treatment program integrates the latest scientific insights and decades of clinical experience, offering a practical and highly effective alternative to standard pharmaceutical treatments. Not only have the methods we recommend been scientifically-validated to perform as well, if not better, than drug-based interventions, and clinically-validated over more than 30 years, they also provide long-term relief by addressing the root cause of vaginal yeast infections.
Each stage is vital, but Stage 4 is where the real transformation happens. This is where you shift from managing infections to building a healthy foundation for lasting gut and vaginal health.
Please share your thoughts or experiences in the comments below—we’d love to hear how this program is helping you on your journey to great health.
Please Follow Through with All 4 Steps
It can be tempting to skip the first step—identifying the cause and stopping repeated drug prescriptions—and jump straight into cleansing and balancing (Steps 2 and 3). However, I strongly urge you not to skip this critical step.
While skipping Step 1 may occasionally work for mild, one-off yeast infections, it will almost certainly fail for chronic or recurring yeast infections. I’ve seen this happen countless times. Addressing the root cause, discontinuing over-reliance on antifungal drugs, and restoring balance is essential for long-term success.
Here are the 4 key steps in brief:
Commit to all four steps for the best chance at achieving permanent relief, and you’ll set the foundation for a lasting solution. Let’s look briefly at each step:
Step 1: Identify The Root Cause
Step 1 is foundational—it focuses on identifying the root cause of the infection and stopping the cycle of symptom management with antifungal drugs. If you suffer from persistent vaginal yeast infections, this step will provide the clarity needed to break free from recurrence.

Step 1. – Identify And Address The Root Cause
The first and most crucial step in overcoming chronic vaginal thrush is uncovering and addressing its root cause.
Many women fall into a cycle of repeated drug treatments, which may provide short-term relief but often worsen the underlying issue.
Pharmaceutical antifungal drugs can disrupt the vaginal microbiome, leaving it more vulnerable to recurring infections.
To break free from this cycle, it’s essential to:
By focusing on this foundational step, you create the conditions needed for lasting relief and recovery.
Step 2: Deep Cleansing
After addressing the root cause in Step 1, Step 2 focuses on thoroughly cleansing the vaginal area and gut microbiota to eliminate harmful bacteria and yeast overgrowth. This step lays the groundwork for restoring balance and can be adapted based on the severity of the infection:

Step 2. – Deep Cleansing
The cleansing phase involves natural remedies such as suppositories, washes, or implants that gently remove pathogens. While this step provides relief from itching and irritation, its primary goal is to reduce microbial and biofilm overgrowth and clearing debris, preparing the vaginal environment for the restorative phase.
Though not as soothing as the balancing stage that follows, deep cleansing is vital for setting the stage for a healthier vaginal microbiome and achieving lasting relief.
Step 3: Microbiome Balance
A balanced and thriving gut and vaginal microbiome creates an environment where harmful yeast and bacteria find it difficult to thrive. To achieve this, I recommend:

Step 3: Microbiome Balance
This rebalancing phase is essential for creating a resilient, self-sustaining vaginal environment that helps protect against future infections.
The balance of your vaginal microbiome is essential for long-term health and protection against yeast infections. In this step, the focus shifts to rebuilding healthy bacterial populations (like lactobacilli) and restoring the vagina’s optimal pH levels.
Step 4: Lasting Health
Step 4 marks the final and most crucial stage of the Yeast Infection Treatment Program. At this point, the focus shifts from managing symptoms to ensuring long-term prevention, helping you maintain a healthy vaginal and gut microbiome.

Step 4: Lasting Health
Chronic vaginal yeast infections often arise from temporary solutions like antifungal creams or medications, which can lead to fungal resistance, disrupt microbial balance, and trigger recurrent infections. Step 4 offers the tools to break this cycle for good.
By addressing underlying causes such as poor diet, high stress, poor hygiene, and antibiotic overuse, and replacing them with healthier, sustainable habits, you can achieve lasting vitality. This stage builds on the foundation set in earlier steps—identifying triggers, cleansing, and restoring balance—ensuring long-term success and health.
Thanks for reading this page. Please leave a comment with your views or experiences, it may help somebody else.

Ultimate Candida Cleanse System
Beat Candida naturally with the complete, science-based system created by naturopath Eric Bakker, N.D. This all-in-one package gives you two downloadable guidebooks plus the Yeastrix Gut Restore Kit — three targeted professional formulas that work together to reset your gut, restore balance, and rebuild healthy digestion.
You get a structured, step-by-step program, professional clinical guidance, and supplements designed to support each stage of recovery. No guesswork. No confusing protocols. Just a clear roadmap and the right tools to help you finally reduce symptoms, rebalance your microbiome, and feel like yourself again. The Ultimate Candida Cleanse System is everything you need to make real progress — naturally, safely, and effectively.

Eric Bakker N.D.
Greetings! I am a naturopathic physician from New Zealand. Although I’ve retired from clinical practice since 2019 after 34 years of clinic. I remain passionate about helping people improve their lives. You’ll find I’m active online with a focus on natural health and wellbeing education through my Facebook page, Reddit page and YouTube channel, including this website.







