
What Is Genital Herpes?
Genital herpes is a common sexually-transmitted infection (STI) caused by the herpes simplex virus. Genital herpes is potentially a highly-contagious chronic infection can be transmitted through direct skin-to-skin contact during sexual activity with an infected person.
What Is Herpes?
The herpes simplex virus (HSV) leads to oral and genital herpes, as well as infections in other parts of the body. While fluid-filled blisters on the skin are a common symptom, many individuals may not experience any symptoms. A simple blood test can determine if HSV is present in the body.
There are two types of herpes simplex virus (HSV) that cause herpes infections:
According to the World Health Organisation, in 2016:

Painful Little Blisters
Many people with genital herpes may not show symptoms initially, which increases the risk of unknowingly transmitting the infection. Symptoms often manifest as painful blisters or sores in the genital and anal regions, accompanied by itching and discomfort while urinating.
The photo to the left is an image of herpes on the crease of the buttocks. Genital herpes symptoms have the potential to recur due to the virus remaining dormant in the body and reactivating periodically.
The diagnosis of genital herpes usually includes a physical exam and lab tests like viral culture, PCR tests, or blood tests to detect HSV antibodies. Although genital herpes has no cure, antiviral medications such as acyclovir, valacyclovir, and famciclovir can aid in outbreak management, symptom reduction, and lowering the risk of transmission.
Genital Herpes Symptoms
Small blisters caused by herpes often appear near the vaginal opening or around the penis. During the initial outbreak, individuals may experience fever, night sweats, swollen lymph nodes in the groin, discomfort, painful urination, and sometimes swelling or redness around the lips and vaginal area.
After the first episode subsides, future flare-ups occur only occasionally. Before a flare-up, the affected skin may become more sensitive, signalling an outbreak. A tingling sensation is often followed by watery blisters, which can be itchy or cause a burning sensation if they burst. Maintaining good overall health can help reduce the frequency of herpes flare-ups.
Most common symptoms include itching, tingling, and the formation of painful ulcers once blisters rupture. Over time, these sores may crust over and heal, they may be accompanied by flu-like symptoms such as fever, headaches, and swollen lymph nodes.
Key Symptoms:
Complications
It’s crucial to inform a doctor if herpes is contracted during pregnancy to prevent transmission to the baby, with cesarean delivery often considered.
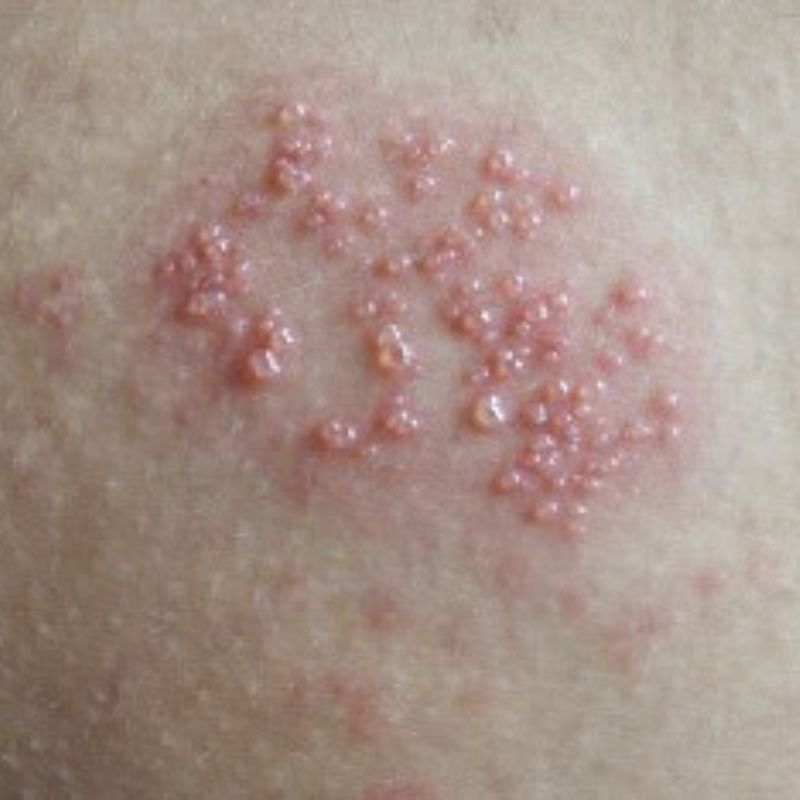
What Does Herpes Look Like?
Genital herpes appears as clusters of small, fluid-filled blisters on the skin or mucous membranes. These blisters can be red, swollen, and painful, eventually breaking open to form shallow ulcers or open sores.
Over time, the sores crust over and heal. Here’s what to expect visually during an outbreak:
Blisters can also form in other areas of the body that come into contact with the infected site, such as the mouth, lips, or face.

How Do You Get Herpes?
Genital herpes is primarily spread through direct skin-to-skin contact with an infected person during sexual activities, including vaginal, anal, or oral sex. The virus enters the body through skin abrasions or mucous membranes, such as those in the nose, mouth, or genitals. Once inside, it integrates into cells and is challenging to treat due to its adaptability.
A person with HSV doesn’t spread the virus from all areas of their body, only from the region where they are infected. The virus is typically shed from the location where it initially entered the body.
For instance, someone with genital herpes transmits the virus through the skin, mucous membranes, and bodily fluids in the genital area. They won’t spread HSV through saliva, unless they also have oral herpes.
If a partner has oral herpes but not genital herpes, the risk of transmission is limited to contact with their mouth or saliva, not their genitals. However, if they have both oral and genital herpes, transmission can occur through contact with either area, depending on which part of your body comes into contact with the infected region.
HSV-1 and HSV-2 can be transmitted via bodily fluids like saliva, semen, and vaginal secretions. The virus is highly contagious and can be transmitted even when symptoms aren’t visible.
Here are the main ways genital herpes can be contracted:
It’s important to note that the herpes virus can still be transmitted even when there are no visible symptoms. Using condoms can help reduce the risk of transmission, but it doesn’t eliminate the risk entirely.
The 3 Main Stages of Herpes Infection

Herpes simplex virus infections progress through three main stages: primary infection, latency, and reactivation. During the primary infection, HSV enters the body and begins replicating in nearby nerve cells. In some cases, people may not experience any symptoms at this stage.
After the initial infection, the virus enters a latent phase, where it remains dormant in nerve cells without causing symptoms. Reactivation occurs when the virus “wakes up,” either causing no symptoms but still shedding the virus or triggering an outbreak with visible blisters that can be easily transmitted to others.
1 – The Primary Infection
A primary infection occurs when HSV first enters your body and begins replicating in nearby nerve cells. If HSV enters through the mouth, it typically infects the trigeminal nerves, while genital HSV infections target the sacral plexus in the pelvis.
The virus travels through the nerves to nearby skin or mucous membranes, triggering your immune system to respond. This causes inflammation, swelling of lymph nodes, and the formation of blisters. Some people, however, may not experience noticeable symptoms and remain unaware they are infected.
2 – The Latency Period
After the immune system manages the primary infection, HSV retreats into nerve cells and enters a “latent” phase. The virus stays in your body, inactive for the most part. However, a few infected cells may occasionally remain active without causing symptoms or outbreaks. This stage can last indefinitely, with the virus lying dormant until something triggers its reactivation.
3 – The Reactivation Stage
During reactivation, the virus “wakes up” and can cause an immune response. I’ve found clinically that one or more triggers occur typically before the reactivation stage. Many people can sense an impending outbreak by recognising warning signs, such as a tingling sensation known as a “prodrome.” During this time, when the skin looks normal but the virus is active, individuals are particularly contagious.
Herpes Outbreak
A genital herpes outbreak refers to the period when herpes sores or blisters appear on or around the genital area. These outbreaks are caused by the herpes simplex virus (HSV), and typically include painful blisters that can break open and become ulcers before eventually scabbing over and healing.
Herpes Flare-Ups
Eventually, the herpes infection settles down, and the individual may experience “flare-ups,” which can occur quite regularly or very rarely. As a warning sign of an impending outbreak, the skin in the affected area becomes increasingly sensitive. For instance, a tingling sensation may precede the appearance of blisters, which can itch intensely and even produce a burning sensation if they rupture.
Therefore, it’s in the best interest of those with herpes to explore ways to improve their health to reduce the frequency of these flare-ups. Moreover, many people with genital herpes typically experience about five to eight flare-ups per year; however, symptoms can vary widely from person to person. Interestingly, as time passes, the frequency of outbreaks often decreases with age.
For women, oral herpes may recur as frequently as monthly, particularly before their periods, while others might only have one or two outbreaks each year, usually triggered by significant stress. Typically, these sores reappear near the site of the initial infection.
Overall, as outbreaks recur, they generally involve fewer sores, which tend to heal more quickly and are less painful. After an outbreak, the blisters typically heal on their own within two to ten days, but the herpes virus remains dormant in clusters of nerve cells until triggered by various factors.
What Triggers a Herpes Outbreak?
Herpes simplex virus outbreaks can be triggered by several factors. Common triggers for both oral and genital herpes include fever, stress, a weakened immune system—often due to medications or underlying health conditions—and hormonal changes, such as those occurring during menstruation.
Specific triggers for oral herpes may include sun exposure, upper respiratory infections, and trauma to the mouth area. Being aware of these triggers can help individuals manage and potentially reduce the frequency of outbreaks.
Key Points About a Genital Herpes Outbreak:
Outbreaks can vary in frequency, with some people experiencing them regularly and others only occasionally. Certain factors, like stress, illness, or a weakened immune system, can trigger an outbreak.
How Long Does A Herpes Outbreak Last?
A genital herpes outbreak typically lasts between 2 to 4 weeks for the first episode. Subsequent outbreaks tend to be shorter, usually lasting about 1 to 2 weeks.
The first outbreak is generally the most severe, while future outbreaks tend to be milder and heal faster.
Anal Herpes
Anal herpes is a form of genital herpes caused by the herpes simplex virus (HSV), typically HSV-2, though HSV-1 can also cause it. It affects the area around the anus and rectum, leading to outbreaks of painful sores and other symptoms.
Symptoms of Anal Herpes:
Anal Herpes Transmission:
Anal herpes is spread through skin-to-skin contact with an infected person during sexual activity, including anal, vaginal, or oral sex. While there is no cure, antiviral medications can reduce the frequency and severity of outbreaks, manage symptoms, and lower the risk of transmission to others.
Genital Herpes Treatment
Herpes treatment focuses on managing symptoms, reducing the frequency of outbreaks, and minimizing the risk of transmission. While there is no cure for herpes, antiviral medications can help control the infection effectively.
Herpes Medication
Different pharmaceutical preparations are commonly availably to help control the symptoms of herpes. By shortening outbreaks, medications can reduce the severity and duration of symptoms during an outbreak.
Some people may wish to take antiviral medications during periods of high stress. By suppressing the virus, daily antiviral medication suppresses the herpes virus, lowering the risk of recurring outbreaks and reduce the likelihood of spreading the virus to sexual partners. The most common medications are:
Acyclovir Side-Effects
Short-term treatment with acyclovir can accelerate the healing of an acute outbreak, and continuous acyclovir therapy is often prescribed for people with frequent recurrences. While this drug can reduce the recurrence rate by 60-90 percent, it can also cause a wide array of side effects, including kidney failure, hepatitis, and anaphylaxis (Gaby 2006).
Managing Herpes Symptoms:
Herpes Flare-Up Advice
During an outbreak of genital herpes, a number of measures can be taken to make the person more comfortable. It is important to boost your immune system and relax more.

Is Herpes Curable?
No, herpes is not curable. Once the herpes simplex virus (HSV) enters your body, it remains there for life. However, the virus can become dormant in nerve cells, and many people may go long periods without experiencing symptoms.
It is essential to comprehend genital herpes and its consequences for sexual health and well-being. Practicing safe sex, using condoms, and having open discussions with sexual partners about STI testing and prevention can help mitigate the risk of infection.
Regular medical check-ups and prompt attention to symptoms can also play a crucial role in managing genital herpes effectively. By raising awareness and promoting safe practices, we can reduce the stigma and spread of this common but manageable condition.
While there is no cure, antiviral medications or treatments can help manage the infection by:
With proper treatment and management, most people with herpes can lead normal, healthy lives.
Herpes Simplex Natural Treatment

Herpes Simplex Natural Treatment
Natural treatment is more than symptom treatment. It’s about improving overall health and establishing any possible trigger or cause.
Common triggers include stress, illness (like a cold or fever), fatigue, sunburn, menstruation, or sexual activity. It is important to establish any triggers or causes of any recurring flare-up of herpes. Have you worked out your own particular trigger or set of causes?
For those dealing with severe herpes, I recommend a natural medicine treatment plan lasting six to twelve months. Traditional medical approaches often label herpes as “incurable,” relying instead on lifelong medication to control symptoms.
However, if you commit to my recommended plan for at least six months, I believe you will experience a significant reduction in flare-ups.
It’s important to remember you cannot “cure” herpes, but you should be able to reduce break-outs or flare-ups significantly. I’ve worked with enough herpes patients in the past to know this for a fact. Here are several treatment recommendations I’d like to make based on clinical experience when it comes to herpes simplex I and II:

The Herpes Diet
A high lysine and low arginine diet is often recommended for managing herpes outbreaks, as the balance between these two amino acids can impact the activity of the herpes simplex virus (HSV). Lysine, an essential amino acid, has been shown to inhibit the replication of HSV, potentially reducing the frequency and severity of outbreaks.
Foods rich in lysine, such as dairy products, fish, chicken, eggs, and certain fruits like apples and pears, can help support this balance. By increasing lysine intake, the body may better suppress viral activity, making it a useful approach for individuals prone to herpes flare-ups.
Conversely, arginine is an amino acid that HSV relies on to replicate. Foods high in arginine, such as nuts, seeds, chocolate, and whole grains, can fuel viral activity and may trigger or worsen outbreaks.
Therefore, reducing the intake of arginine-rich foods while increasing lysine-rich ones can help manage herpes symptoms. Combining this dietary approach with overall stress management and a healthy lifestyle can create a more effective strategy for reducing the impact of the virus.
Lysine-Rich Foods
Eat More of These Foods
Arginine-Rich Foods
Eat Less of These Foods

Ultimate Candida Cleanse System
Beat Candida naturally with the complete, science-based system created by naturopath Eric Bakker, N.D. This all-in-one package gives you two downloadable guidebooks plus the Yeastrix Gut Restore Kit — three targeted professional formulas that work together to reset your gut, restore balance, and rebuild healthy digestion.
You get a structured, step-by-step program, professional clinical guidance, and supplements designed to support each stage of recovery. No guesswork. No confusing protocols. Just a clear roadmap and the right tools to help you finally reduce symptoms, rebalance your microbiome, and feel like yourself again. The Ultimate Candida Cleanse System is everything you need to make real progress — naturally, safely, and effectively.

Eric Bakker N.D.
Greetings! I am a naturopathic physician from New Zealand. Although I’ve retired from clinical practice since 2019 after 34 years of clinic. I remain passionate about helping people improve their lives. You’ll find I’m active online with a focus on natural health and wellbeing education through my Facebook page, Reddit page and YouTube channel, including this website.






